Sorry we left everyone hanging…we just needed a day or two to catch our breath.
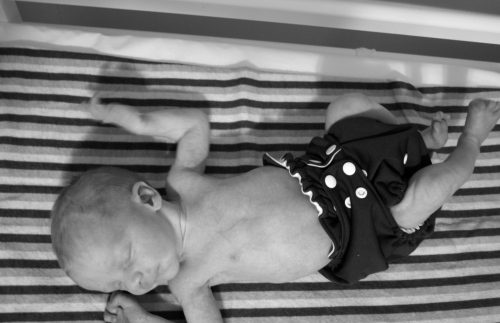
Friday; Samuel Montgomery was lifted out at 7:41am, February 17th. He is a long, lanky, little guy; 5 Pounds, 12 Ounces, 19 and3/4 inches long. Cute as he can be.

I was able to see his body from where I was while capable hands quickly assessed him. They put a little mask over his mouth and nose and manually pumped him with some oxygen*during those first minutes. I won’t forget the NICU nurse turning after a couple of moments to gently inform us that he was having some difficulty breathing and that she would need to take him with her.


No, this wasn’t what we had expected. Because they had to cut through the placenta to get to him, a good bit of the blood that was supposed to go into his body through his cord did not make it to him, so poor little Sam just had to ramp up his breathing to get the blood he was left with up to his brain. He achieved this goal and kept his oxygen levels right where they needed to be. It’s just that he had to work extra hard to get them there.
Later tests showed that he had lost at least 45% of his blood in just those first minutes. He received a blood transfusion within a few hours and has been working quickly to get back on track ever since. He had his Daddy right by his side nearly every minute of that first day- his silent cheerleader. He is doing really well.


Brian took solace in knowing that I had my own cheerleaders with me as he stayed with Sam. Back in the recovery room after being glued back together, I had my own little battle with some blood loss. My mom found herself right in the midst of things as the post-placenta previa bleeding presented my caretakers with several options. Because the placenta had been located in the lower part of my uterus, it lacked the solid tension it needed to contract and quit the bleeding now that the placenta was gone. Basically, it was like an open wound in need of pressure. One of three things could have happened to stop the bleeding: Pressure could be placed on the “wound”; they could wheel me back into the OR and perform a D&C to suction everything out; or they could need to perform a hysterectomy in order to finally get the bleeding under control. I got away with the very best scenario and it worked like a charm…I’m just going to envision balloons differently from now on.
My nurses, Tara and Anna, Midwife Meredith, and Dr. Allen all worked quickly and so efficiently together (my mom has shared her admiration at their work with me from her vantage point) to use what is called a Bakri Balloon which they “installed” and filled with water. Once it was filled, it placed pressure where it needed to be placed, from the inside, and started working right away. Thank you, inventor of the Bakri Balloon. You may have saved me my uterus. I lost 1600 ccs initially, then about 50 ccs per hour after that for the next few hours, then it tapered off quickly and I am doing just fine…taking some extra iron. That little hiccup, combined with the effects of epidural drugs and my own crazy hormones, made for a rough day Friday.
One thing I absolutely admire about the caretakers here is that they don’t let anything get in the way of a mama who needs to see her new baby. Once my self-assessment was complete and I had determined that I was perfectly fine, I called Tara to let her know that I was ready to be-bop down the hall to the NICU and just swing by and pick up my little cuddle bug…or something like that…
She came faithfully and without questioning my desire one bit. I had about fifty cords coming out of me in different directions. We got those sorted and I slowly sat up. I barfed a bit and we continued. I got into the wheelchair and we made our way to the NICU. Through the first door and into the washroom which leads into the NICU, Tara waited patiently while I barfed some more and one of the NICU nurses came out to help console me. I am really thankful that there weren’t other parents in the washroom to witness my new hobby I have decided to call “Puke-Bawling.” It’s where you bawl because you are so upset that you are puking because all you want to do is see your baby.
I finally made it to his bedside. Brian explained everything he had been through very carefully. His transfusion was complete and he had pinked up and taken the blood well. He had a little tube in his nose, but he never needed actual oxygen. All it was doing was pumping a bit of warmed, humidified air just to help his lungs inflate better and get out any amniotic fluid. He had a tiny orange tube coming out of his mouth and taped to his chin, and a whole bunch of sensors. I was in a fog, couldn’t keep my eyes open, and didn’t want to vomit on my child, so Tara wheeled me back.
Throughout the day, we had a great little support team. Aunt Suzanne shared a graceful balance between her niece and nephew. She and Harper spent morning time together and she and Brian and Sam hung out for a long time in the NICU that afternoon. She brought back videos to show me. Cary drove down early so she could be with Harper. She had learned about a playground right up the street and she took Harper there in the stroller. She and Harper were right by my side when the neonatal doctor came in to deliver the status of Sam and the confusing news that his stay in the NICU could be much longer than I had expected. Cary and Harper both consoled me when I burst into tears. Harper patted my knee and brought me jello and it really did make me feel better…that girl…just don’t even get me going…I love her.
Mom and Dad were right there too, giving attention to me, Sam, and Harper throughout the day. Brian’s parents had to attend a funeral in West Virginia and should be getting in to visit today or tomorrow. Sally and Ina were still in town and got to sneak in and see Sam. I can’t really recap the day justly. I was out of it.
The good part about the closure of Friday was that I got to wheel back in to see Sam at around 10pm, nausea free. I got to look at him forever and kiss him. It was hard to fall asleep thinking of my baby over there without us. I used a good bit of tissue throughout the night.
Saturday was a new day, though; a day that began with a visit from Dr. Smith who removed my balloon, catheter, and IV port all at once. Freedom. A shower. Then a disappointing wait once we arrived at the NICU, cord free, to see Sam. The doctor had just gotten there to do rounds and they won’t let anyone in while he does this. We waited.
Finally we got to him. I got to hold him! He is amazing. They were weaning him from his air tube and he had gone from a 5.0 the night before to a 3.0. (meaning the amount of air they were giving him) and was headed quickly in the right direction. Harper and Nana arrived and Brian took Harper to the playground while Nana sat with me and Sam. I have not been able to feed him yet because of the stress on his kidneys, liver, and his other less vital organs while he was getting all that blood to more important places. The doctor wants to see these acting better before he lets him nurse. This has been a little hard for me to deal with. It feels like I’m starving my child…but we’re getting there. Possibly today, they say.
As the day moved on, I gained more and more comfort in the situation. The nurses with Sam are so good and now leaving him doesn’t seem so hard. Papa and Brian had a good visit with Sam in the afternoon, and I got special visitors; Aunt Gail and Unckie Roy drove all the way from south Georgia just to see me. Later, Carolyn and Francois came for a long visit and brought Sam the most beautiful giraffe.
Brian and I returned to Sam’s bed last night and both got to hold him skin to skin. I loved that his nurse, Katie, thanked us for coming in and told us we made Sam’s night. As if he didn’t make ours.



Today it is Sunday; We have just had the best news of all! Sam’s nurse, Laura, mentioned that they would be getting full later today or early in the morning with a transfer baby. She thought Sam would be a good candidate to be transferred to Pediatrics. I was confused at first because I thought this meant that he would be taken to a different nursery, but she said someone had to be with him all the time and she wasn’t sure I could be discharged. We took it as something to think about.
When we got back to Mother/Baby, we gave all our nurses (they are all our nurses- remember how long I’ve been here?) the update and the news that he was being considered. They all lit up and told us that it probably meant he would have his own room and I would be in the room with him, but if I were discharged, I would just be like Sam’s guest in his room….same room! No nursery! He would get to meet his big sister! I’m so excited right now. We wheeled down the hall and immediately called Laura to tell her that I could likely be discharged today and go with him, to PLEASE keep us in mind as the candidates!
…and that’s where we are. I’m beaming right now. Everyone, keep your fingers crossed that we go to Pediatrics today! Incredible things have happened in two and a half days. We’ve caught our breath and we’re moving forward.
________________________
*They did not manually pump, Brian says. What do I know? I was craning my neck from an operating table being sewn and glued, and I was looking through scrubs and elbows.